'˜Third option' put forward to save Horton maternity unit
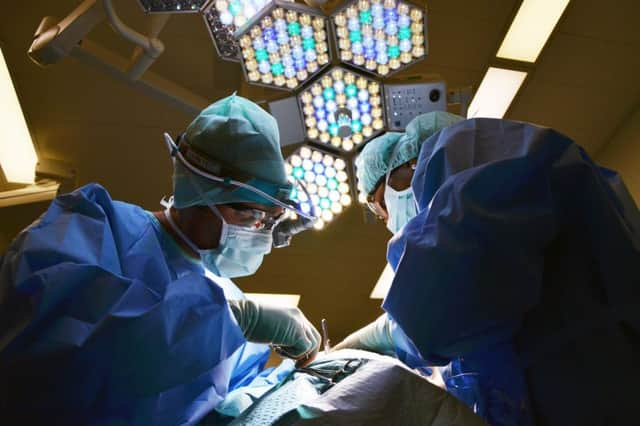

The maternity hospital is due to be downgraded to a midwife-only unit starting on October 3. Midwives believe the remaining Horton service would survive only a few months.
Experts have drawn up a business case for a new idea to keep the maternity unit active while offering dedicated training to Oxford staff.
Advertisement
Hide AdAdvertisement
Hide AdIn the plan, the John Radcliffe Hospital would send its routine, planned Caesarean section births to be carried out in Banbury’s fully kitted-out delivery suite theatres.
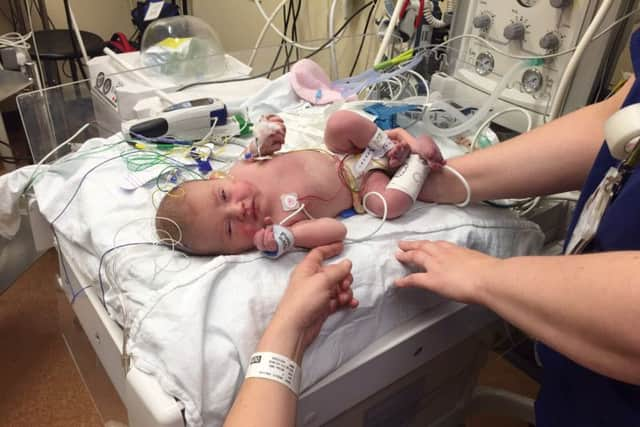

Having the operations done here would
- enable the post natal ward and Special Care Baby Unit to be maintained
- help protect the future of the children’s ward
- ease anticipated pressure on JR staff and obstetric and gynaecology facilities and


- prevent unnecessary expense hiring a portable operating theatre at the JR to house gynaecology ops to make way for planned Caesareans.
Advertisement
Hide AdAdvertisement
Hide AdThe experts have cited parts of an OUHFT contingengy plan that admit to a worrying logjam of births at Oxford.
The infrastructure is already in place in Banbury and, importantly, allowing the Horton to be kept in use would
- prevent inevitable resignations of midwives and SCBU staff being forced to transfer their work to Oxford and
- facilitate the smooth return to full consultant-led maternity as soon as sufficient doctors have been recruited - a move the trust has assured the Board it wishes to make.
Advertisement
Hide AdAdvertisement
Hide AdThe business case says the OUHFT contingency plan describes a ‘major challenge facing OUHFT’ being emergency theatre time, post-operative recovery beds, anaesthetists and theatre staff’.
The experts’ plan claims to eradicate concerns over staffing, availability of beds, weekend gynaecology operating lists and delivery theatre suite availability at the JR.
The ‘third option’ suggests the Horton maternity unit would undertake up to four Caesarean section operations per day, seven days a week, potentially 28 a week, easing pressure at the JR immensely.
One of the experts said: “Staff at the JR have already expressed concerns to management about staffing levels, sickness levels and infrastructure for the present birth rate at the JR, before the predicted 19 extra births per week from October 3.”
Advertisement
Hide AdAdvertisement
Hide AdBecause of the comprehensive nature of the Horton unit, all midwives are already fully trained in all aspects of delivery, including theatre nursing, all categories of Caesareans, post operative and post natal care, so no extra staff or training would be necessary.
The Care Quality Commission scored Banbury over the JR for patient satisfaction and the experts believe patient experience would also be maintained by this third option.
“This third option will complement the midwife-only unit, save the trust money, utilize and maintain current systems of operation and ensure swift and smooth reopening of the full Horton Maternity Unit once middle grade doctors are employed,” they say.
“It will also help repair the lack of trust in OUH displayed at the recent public meeting at St Mary’s Church, Banbury.
“It may also help to retain staff at the Horton and JR.”
Advertisement
Hide AdAdvertisement
Hide AdThe plan would also reduce costs on bank staff needed in the event of expected resignations and disruption to operating lists at the JR which would help the trust avoid expensive fines for missing targets.