From hospice to response centre and back: Katharine House Hospice’s COVID-19 experience
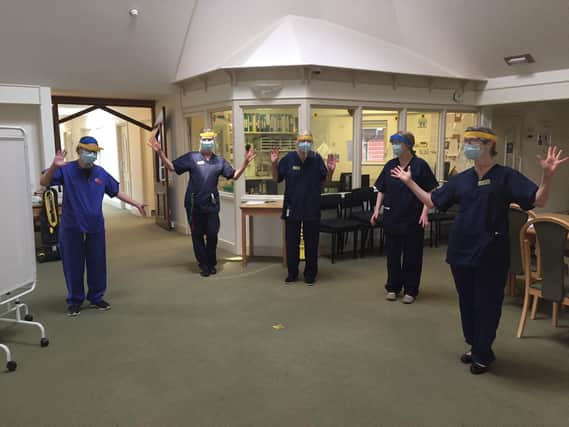

Katharine House Hospice in Adderbury has been greatly touched by the outpouring of help from people when the hospice gave their support to the NHS by becoming a temporary response centre to take patients with a COVID-19 diagnosis.
Katharine House Hospice was faced with a rapid change when COVID-19 hit the UK. Over one weekend in April, plans to turn it into a COVID response centre were put into place.
Advertisement
Hide AdAdvertisement
Hide AdMark Wilson, facilities manager, said: “We had to rise to the urgent challenge of turning our 10-bed inpatient unit into a 26-bed facility – all within the matter of weeks.


"Offices, patient lounges and even the chapel were converted into temporary wards. Beds were brought in and carpets were replaced with floor tiles, and plumbing was installed. We had no idea how many patients would be coming in, but we knew we had to be ready to respond to the needs of the community.”
The hospice had exactly the right facilities to help relieve the pressure that the pandemic was placing on local healthcare. The hospice healthcare professionals, staff and volunteers came together to do whatever it took for the transformation from hospice to response centre.
Helen Fletcher, head of the inpatient unit, said: “I remember the day I contacted every member of my team to tell them about the changes we were proposing, how it might look and feel and whether they would be prepared to work in an environment where we would be caring for patients with COVID-19. Every one of them said yes, we want to do this.”
Advertisement
Hide AdAdvertisement
Hide AdAngharad Orchard, chief executive of Katharine House, said: “I’m so proud of the contribution our doctors, nurses, staff and volunteers have been making in circumstances we could never have imagined at the start of this year. For most, this meant working long difficult hours, and for some the need to live away from home to protect their young families.”


New ways of working
Not only was the hospice coping with the health crisis in the community they support, but staff and volunteers were experiencing the same worries and difficulties as everyone else in the community combined with learning to work in new ways.
The Living Well and Community Nursing teams continued to reach out to the community, but now in different ways.
Lydia Brook, head of living well, said: “We’re used to seeing a steady stream of visitors dropping into our sessions to take part in activities, get a bit of advice or to enjoy the company of others in our lovely, sunny lounge. But then with lockdown, all this changed overnight and we had to find new ways of supporting people remotely.


Advertisement
Hide AdAdvertisement
Hide Ad“We’re regularly speaking to people on the phone, encouraging them to take part in home-based crafts and activities to keep them busy and we’ve been producing a regular newsletter to keep everyone feeling connected to Living Well. We even started running exercise and breath meditation classes by video. The important thing is for us to help people remain as happy as they can while they’re unable to come into the hospice and that they continue to feel connected and supported by the Living Well team during this time.”
The Community Nurse Specialist (CNS) team played an important part in setting up and running a 24/7 Palliative Care Resource Line to support healthcare staff working on the frontline.
This was staffed by the CNS team at Katharine House together with colleagues from Sobell House and Sue Ryder. Its purpose was to give palliative care advice to care homes and GPs who may be faced with rapidly deteriorating people due to COVID-19.
Katie McGovern, one of the CNS team, said: “We’ve also been providing continuing support to our patients in the community. It’s all been possible by phone, but I think we all hugely value face-to-face contact with patients, and are relieved that we can visit more now – even when we have to wear PPE. Patients are very understanding when we turn up at their homes in scrubs, gloves and masks.


Advertisement
Hide AdAdvertisement
Hide AdOther teams were also affected by the change into a COVID response centre. The housekeeping team, for example, had to take on additional infection control and significant amounts of deep cleaning. But staff members from other teams stepped up to help in this new work environment.
Cherida Plumb, the hospice’s community and event fundraising manager, said: “During lockdown I worked alongside our team in the Inpatient Unit (IPU) to help cover staff shortages while colleagues needed to stay away from the hospice to shield themselves or protect loved ones. I was more than happy to put myself forward to help the housekeeping team.
"I was quickly trained up in the very thorough process of cleaning the IPU. Since then I’ve been lending a hand whenever needed. It has been sometimes scary, but I’m so proud to have been able to support colleagues through some very hard times and do my bit to help patients and their families.”
The return to hospice care
At the end of July, Katharine House returned to its original 10 beds and continued care for in-patients with specialist palliative care needs.
Advertisement
Hide AdAdvertisement
Hide AdHowever, the effects of the pandemic remain apparent within the building. The clinical staff remain in PPE and although the painful decision to have no visitors has been changed, the numbers remain restricted. More ‘normal’ working hours have resumed, but the building remains COVID-secure.

Angharad Orchard said: “The impact of the pandemic on hospice funding has been fundamental. Like everywhere, the hospice shops had to be closed and many of our community fundraising events were cancelled or delayed, including the Midnight Walk, the hospice’s annual main fundraising event.
"Then there was closure of Open Gardens for Katharine House, and the supermarket collections and collecting boxes had to be stopped - all these sudden changes has seen a significant shortfall in funding for this year.”
While the hospice was operating as a response centre for COVID-19 patients, it received financial support from the NHS, but that has now finished and Katharine House once again faces significant financial deficit.
Advertisement
Hide AdAdvertisement
Hide AdThe hospice needs urgent funds to ensure it can continue to serve local people with the care they need, when and where they need it.
It costs £13,000 per day to run the charity - or £8/minute - and only 25 per cent of the hospice’s funding is provided by the government.
Angharad added: “Our sincere thanks go to everyone who made a financial gift, donated personal protective equipment (PPE), provided tablets so patients could keep in touch with loved ones, and to all of you who have supported us in many other ways."
If you wish to find out more about Katharine House’s work, make a donation or join in on one of their fundraising events, go to their website at www.khh.org.uk."We hope that you will feel able to continue to support us in the months ahead in the invaluable work that we do here at Katharine House Hospice.”