Cancer warning over skin bleaching treatment
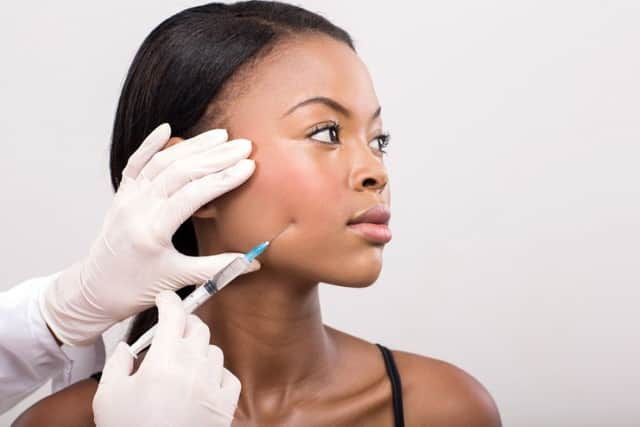

Leading dermatologists issued the warning as skin whitening is becoming increasingly popular among both young women and men.
Dr Ophelia Dadzie, consultant dermatologist at The Hillingdon Hospitals NHS Foundation Trust,, told the BMJ: “Skin bleaching is a cosmetic procedure that involves lightening constitutive skin colour, and one such agent used is glutathione, an antioxidant that can be administered orally or intravenously.”
Advertisement
Hide AdAdvertisement
Hide AdDr Dadzie said there has been a shift from using skin lightening creams to intravenous treatments.
She said: “It is through my patients that I learnt about the increasingly use of intravenous glutathione for skin lightening.
“I cannot explain why this particular practice is on the rise.
“I have a special interest dealing with skin and hair problems in the UK’s ethnic minority groups and I have seen skin bleaching in both men and women, although in my experience it is predominantly in women.
Advertisement
Hide AdAdvertisement
Hide Ad“It is a practice taking place in those with darker skin tones, those of African, Afro-Caribbean and South Asian origin in the UK.”
Dr Dadzie said that treatment is usually provided at beauty salons and can be administered by non-medical practitioners.
“The cost of this treatment can be very high,” she said. “Yet there is no explicit approval for the use of glutathione for skin bleaching.”
The practice can come with an array of nasty side effects, said Dr Dadzie.
Advertisement
Hide AdAdvertisement
Hide AdIt can cause toxicity of the nervous system, kidney and liver; transmission of infections such as HIV; headaches; rare skin conditions and even skin cancer.
Dr Dadzie said: “There is a lack of authoritative public health information in the UK about the efficacy and safety of this practice.
“No published clinical trials have evaluated the use of glutathione for skin bleaching, and no published guidelines exist for appropriate dosing regimes, or guidance for treatment duration.”
In contrast, both the US Food and Drug Administration (FDA) and the Dermatology Society in the Philippines - where the practice is common - have issued advisory warnings about the treatment.
Advertisement
Hide AdAdvertisement
Hide AdDr Dadzie added: “Clear public health information and advisory warnings in relation to this practice - from governmental agencies such as the Medicines Health Regulatory Agency - are needed in the UK.”