Patients may have to isolate before planned operations at Banbury and Oxford hospitals
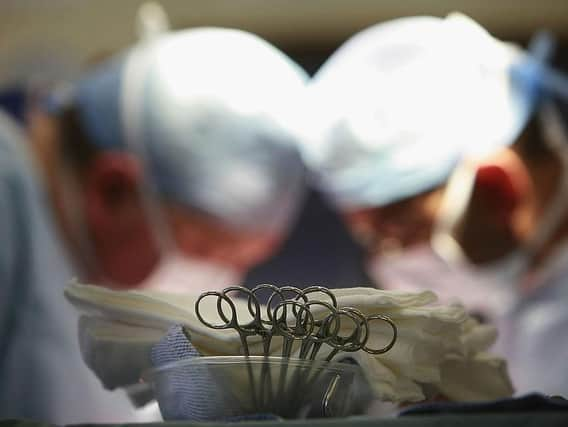

According to new guidelines they should then fully isolate from the time of their Covid-19 test. Those who are vulnerable will need to self-isolate before admission for 14 days 'where possible'.
These are the latest rules for those being included in the resumed programme of planned surgery at the Oxford University Hospitals NHS Trust (OUH).
Advertisement
Hide AdAdvertisement
Hide AdThe guidance was changed by government last week from a position where patients faced a full 14-day isolation before being allowed to hospital for a procedure and another 14 days afterwards.
However it became clear that numerous people would have to decide whether to go ahead with a necessary operation and foregoing pay. Statutory sick pay would not be available for these periods of isolation.
The updated guidance now says that patients should observe strict social distancing for 14 days and have a Covid-19 test three days before admission - isolating from then until being admitted for their operation.
In a statement the OUH said: "National guidance has changed for people who are attending hospital for surgery.
Advertisement
Hide AdAdvertisement
Hide Ad"For planned procedures, patients should follow comprehensive social distancing and hand hygiene measures for 14 days before having planned care. Patients having planned care involving any form of sedation should follow these same social distancing measures and are advised to have a COVID-19 test within three days before their procedure and then self-isolate from the day of the test until the day of their treatment.
"More vulnerable patients will still be advised to self-isolate for 14 days where possible. On discharge, only patients with a positive COVID-19 diagnosis need to self-isolate for 14 days.
"National guidance is subject to change as the situation evolves and we look to follow it wherever possible."
The trust said patient and staff safety is at the forefront of its plans. Reinstating services in a safely takes time and consultants are giving priority to patients who have the greatest clinical urgency.
Advertisement
Hide AdAdvertisement
Hide Ad"While we may be past the peak of the Covid pandemic, the impact is still being felt across the NHS," said a spokesman. "To help mitigate this, we are working closely with our partners to maximise all available capacity for our patients. We are also continuing to work with the independent sector which has provided much-needed additional capacity."
The National Institute for Clinical Excellence (NICE) guidance warns that local and national coronavirus outbreaks may force hospitals to change surgery schedules.
It says: "Providers should be responsive to local and national prevalence so that services can be stepped up or down. (They should) maintain effective communication and collaboration with regional NHS England and Improvement and local public health teams to determine the current prevalence of COVID-19 in their local communities."
* Hospitals across the country have a huge backlog of planned surgery that has been put on hold during the coronavirus crisis. A consultation is underway to extend restrictions on various procedures to cut 350,000 'spells of activity' and 'improve' demand.
Advertisement
Hide AdAdvertisement
Hide AdAccording to Health Service Journal the proposed restrictions to 31 procedures include some colonoscopies and endoscopies, X-rays for frozen shoulders, MRI scans for arthritic hips and some chest X-rays, as well as restricting surgery for slipped disks, groin hernias and knee pain.